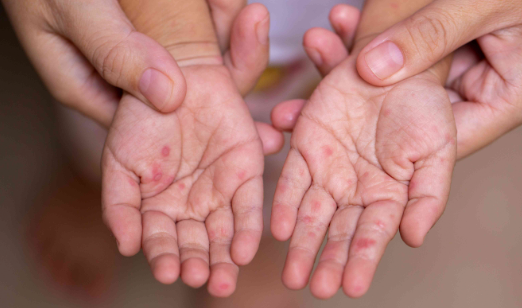
A Hidden Surge: Hand-Foot-and-Mouth Disease Finds New Momentum in the U.S.
In an autumn when flu and cold season often dominate headlines, a less-heralded illness is quietly gaining ground across the United States: Hand‑Foot‑and‑Mouth Disease (HFMD). What begins as a mild viral ailment in most cases is drawing attention because of its sudden uptick among children and the ripple effects it carries for families, day-care centres and schools.
Health officials in several states have reported a noticeable rise in HFMD cases. In regions such as the mid-Atlantic and parts of the Midwest, emergency department visits for children under five presenting with typical HFMD symptoms have climbed compared to recent years. The increase is layered: a mix of seasonal dynamics, greater viral spread in indoor settings and perhaps lower population immunity following the disruptions of recent years. Although primarily a childhood illness, the implications extend beyond a run-of-the-mill virus.
HFMD reveals itself with deceptively simple signs: a fever followed by sore throat, often accompanied by painful red spots or blisters inside the mouth and on the palms of the hands and soles of the feet. Infections can spread rapidly in day-care centres, schools and households where close contact, shared toys and high-touch surfaces are the norm. The causative agents are enteroviruses — especially the coxsackievirus family — which spread through droplets, saliva, blister fluid and even stool. This combination of factors makes containment in communal settings more challenging than one might assume.
The tone from paediatricians and public-health experts is one of cautious concern rather than alarm. Most children recover within a week to ten days with no lasting effects, but the burden lies in supporting a child through throat pain, reluctance to eat or drink, and the parental juggling act that comes with keeping them home, hygienic and comfortable. The larger worry is how the spread might back-up day-care attendance, overwhelm small clinics in certain hotspots and even tack on extra stress to families already stretched.
Prevention has become the watchword. The standard playbook is simple but effective: frequent hand-washing (especially after diaper changes, bathroom visits or contact with a sick child), disinfecting common surfaces, avoiding shared utensils or towels, and keeping children home until they show signs of improvement. Education efforts are pointing heavily at parents, child-care providers and school administrators to recognise early signs — a sore throat here, a rash there — so that transmission chains can be interrupted.
Yet the rise of HFMD also reflects the changing context of viral illnesses. With many childhood viruses less exposed during pandemic restrictions, immunity patterns shifted. Combine that with younger children returning to group settings and increased indoor time, and you have an environment more conducive to outbreaks of viruses that had been languid. It’s a reminder that public-health preparedness isn’t just about the big headline pathogens but also those older familiar viruses that find new life when social conditions change.
For the pediatrician, the message is clear: track trends, warn parents about symptom patterns, counsel on hydration (especially given painful mouth sores that reduce eating or drinking) and emphasize rest and isolation of affected children. For parents, the emotional radar must be tuned sharp: when a child develops mouth sores along with a rash on hands or feet and a fever, HFMD must enter the differential diagnosis rather than be dismissed as a minor cold or rash.
Crucially, while HFMD is generally benign, complications — although rare — can occur. Dehydration, secondary infections or, in very rare instances, neurologic involvement demand vigilance. When symptoms persist beyond a typical window, show signs of progression or when a child seems unusually drowsy or refuses fluids, escalation to medical care is prudent.
In this episode of viral resurgence, the broader lesson is that outbreaks don’t always arrive with a bang — sometimes they build quietly, riding on existing infrastructure: day-care halls, shared toys, small classrooms, and children who bring the virus home. Addressing them isn’t simply about medical intervention but about social hygiene, communication and community awareness.
As U.S. public-health infrastructure and caregivers mobilise around this uptick, the hope is that HFMD will remain a manageable wave rather than becoming a disruptive storm. But with the environment shifting, vigilance must be sustained. In a country always ready for the next big public-health challenge, sometimes the quiet ones prove the most instructive.